Opinion
The New Mpox Clade Exposes International Health Law as a System Without Enforcement -By Fransiscus Nanga Roka
And that is the highest indictment of where we are: Even so, together with a legal order that fails to enforce collective protection from global biological emergencies does not serve humankind. Managing collapse, while maintaining the illusion of control.
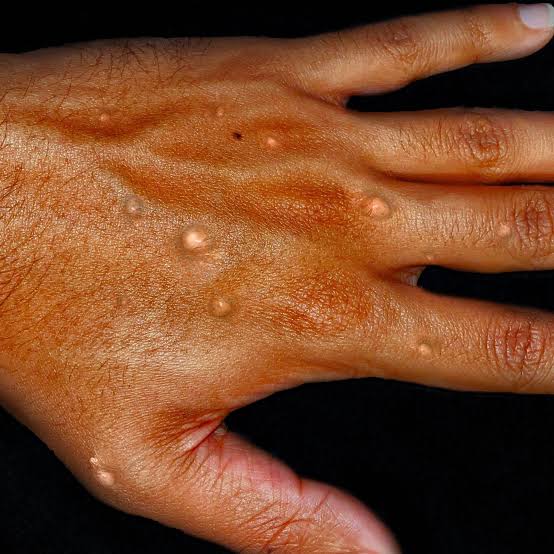
The rise of a new Mpox clade is not just a biomedical alarm system. It is a legal indictment. This talk of “global preparedness,” international cooperation, and health security masks an uncomfortable truth: as it exists today, the field of international health law remains structurally unable to enforce its obligations.
Mpox is evolving biologically. International law, in turn is held hostage to diplomatic posturing. The world has operated for years under the belief that global health governance is equipped with appropriate legal tools and mechanisms to prevent, diagnose and contain transnational outbreaks. With the World Health Organization, International Health Regulations (2005), global pandemic preparedness frameworks and numerous international declarations it will seem that protection is coordinated. But the emergence of a new Mpox clade has revealed what many governments would rather not acknowledge: that in reality, unlike civil and criminal law where sovereignty does no exist, global health is largely founded on political will over legally binding obligations.
The International Health Regulations (IHR) were created to facilitate fast reporting, transparency, surveillance collaboration and organized responses in times of public health emergencies. Conceptually, they are one of the most important hard law tools in global health governance. This sounds nice in practice, but they carry a fatal limitation: it almost never results in significant punishment for lacking compliance.
States may delay disclosure. Governments may underreport risks. Vaccine nationalism may prevail. Medical resources may be hoarded. Surveillance might continue to be perilously underfunded. But penalties for failures at such will be almost always political rather than legal. Without the potential for enforceability, there is no regulation. It is aspiration.
This structural flaw is precisely demonstrated through the new Mpox clade. Nations already having fragile health systems are still faced with the challenges of poor laboratory capabilities, weak genomic surveillance, limited vaccine access and delayed containment capacity. Wealthier states, in the meantime, ramp up preparedness only when cross-border transmission is perceived as a direct threat to their own populations. This means a two-speed global health order: some lives only become urgent when contagion reaches the economically powerful West. This inequality is not a side effect of the system. It is embedded within it. Global health legislation calls on solidarity time and again, yet allows intolerable imbalance of access to medicines across the globe. Low Income Economies are often made to feel that they should communicate fast reporting and pathogen transparency during infectious disease emergencies without equitable guarantees of medical assistance, technology transfer or access to countermeasures. This creates a system that takes cooperation from vulnerable states while maintaining the power advantages of strong ones.
Stay ahead with the latest news in health policy and practice. Defacto inequality in humanitarian clothing. Compounding the iffy legal grounding of their present structure, is that we live in times where biological risk posed by stealthy pathogens accelerating. Emerging diseases are becoming more common and complex due to climate change, environmental destruction, rapid urbanization, world-wide travel & communication across borders, conflict and antimicrobial resistance. Outbreaks should be understood not as exceptional crises in their periodicity, but rather systemic realities we must learn to live with. But international law still resorts to soft compliance mechanisms that are more in keeping with diplomatic wishes than planetary needs.
The contradiction is staggering. The virus traverses continents in days, but international agreement and hence enforcement of the law it espouses remains hostage to state consent subject to geopolitical/diplomatic bargaining power in a climate that encourages institutional timidity about bold or activist moves.
This paradox is reflected in the WHO itself. It would be guided by global health response But with no independent enforcement powers over sovereign states. Sure, it can issue recommendations and proclaim states of emergency; but its non-binding nature alone means that compliance cannot be mandated in the same way as other areas of international law. In short, the institution that exists to protect global public health is structurally dependent on the voluntary cooperation of exactly those actors whose failures could exacerbate epidemics. Well, no security architecture can operate optimally in such conditions. Of equal concern is the political bias embedded within responses to outbreaks. Diseases in neglected parts of the world often fail to maintain sustained global urgency unless and until transmission threatens wealthier countries. We saw this pattern during Ebola. It resurfaced during COVID-19. It is manifested once more in the global response to Mpox.
The pattern is brutally obvious: certain outbreaks are considered a regional misery until they become geopolitical inconvenience. Such pick and choose urgency undermines the moral authority of global health law. A system of containment by definition turns public health into a hierarchy of human value. Its legal consequences are much deeper than the institutional weakness. All Human Rights Law responsibilities of states globally include one or the other, right to health, non discrimination legal access to medical care and scientific progress international cooperation. And yet, during health emergencies of the magnitude faced by our planet very often these obligations are placed behind short-term economic interests, border relations politics, pharmaceutical monopolies and nationalistic ploys.
In other words, the issue is no longer just legal insufficiency. It is the legal normalization of avoidable injustice. The recently recognized Mpox clade must catalyse a radical rethink of global health governance. The status quo of international health law as norms without sanctions has to come to an end. Recurrent outbreaks with transnational impact demand legally binding transparency standards, enforceable cooperation obligations, equitable vaccine responsibilitie, independent investigations of outbreak origins and legal mechanisms for accountability in case the origin was wilfully obfuscated or neglected.
Without enforceability, preparedness becomes rhetoric. Without equality, solidarity becomes fiction. They become a ritualistic lingua franca of international health law over far too predictable human suffering1 where accountability is the exception, not the norm.
Emerging outbreaks are commonly called by the world as an “unexpected crises”. Yet Mpox ιmakes a much uglier argument: the biggest threat today is not that pathogens could turn rogue. It is the height of political failure, which you could easily anticipate.
And that is the highest indictment of where we are: Even so, together with a legal order that fails to enforce collective protection from global biological emergencies does not serve humankind. Managing collapse, while maintaining the illusion of control.
Fransiscus Nanga Roka
Faculty of Law University 17 August 1945 Surabaya Indonesia